AudioVisual Recording & Debriefing Systems for Healthcare Simulation
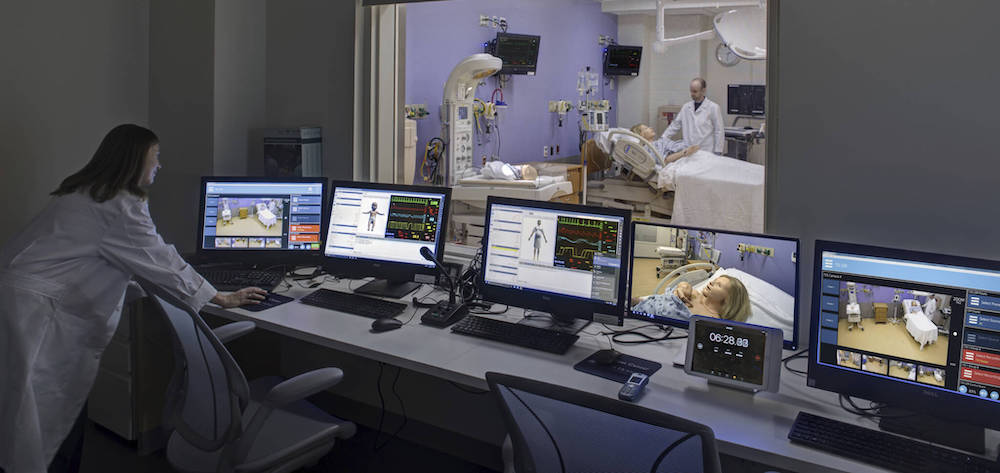
Medical Simulation A/V Recording Systems are specialized Learning Management Solutions used to display real-time clinical simulation activities to non-participating learners as well as to playback the recorded simulated learning experience for debriefing purposes. These unique learning management software systems are used for education and training purposes in healthcare simulation programs around the world. Such simulation based education (SBE) debriefing systems are now regularly robust cloud-based platforms which enable educators to stream, record, debrief, and annotate educational learning activities for mobile in-situ professionals, classroom sim lab students, and clinical research projects. Note that these Learning Management Systems for simulation audiovisual engagements, is different from AV Integrators or AV System Designers, who are usually experienced audio video hardware experts who plan, design, install, and maintain audio and video hardware equipment. While you can learn more about How A/V Recording Systems Work in Healthcare Simulation, here below we summarize the key corporations offering leading nursing simulation, surgical simulation, or otherwise simulation in healthcare programs with the latest in AV recording systems for contemporary clinical education and medical training!
CAE Healthcare: CAE Healthcare, a division of Canadian-based CAE (NYSE: CAE), is among world leaders in developing cutting-edge healthcare simulation learning tools for today’s professional healthcare providers. The company strives to deliver educational tools that best help healthcare professionals provide safe high quality patient care. CAE Healthcare has an extraordinarily vast area of simulated products ranging from manikins, interventional and imaging systems, and AV recording debriefing / Learning Management Systems.
CAE LearningSpace is a powerful simulation center management solution for medical schools, nurse education programs, allied health and hospital-based simulation programs. The scalable healthcare education platform is user-friendly, web-based and secure. Invest in LearningSpace to gain a 360-degree view of your simulation training environment performance and educational outcomes. Your faculty will deliver more effective video-driven improvement with integrated patient data and facilitator’s notes. Your center director will provide objective, data-driven assessment tools while managing your healthcare simulation training environment more efficiently anytime and from anywhere.
Sponsored Content:
CAE LearningSpace Experience is a simplified solution for simulation video capture and debrief. LearningSpace Experience/Replay is easily adaptable within a fast-paced healthcare environment where standards and practices are rapidly evolving. The user-friendly system allows clinical teams to practice new safety protocols and gain instant feedback.
SimulationIQ from Education Management Solutions: Education Management Solutions (EMS) and their brand SimulationIQ is a leading healthcare simulation company which provides audiovisual recording debriefing systems, learning management systems, A/V design consulting, online learning systems, counseling training systems, virtual patient simulations, as well ROI and competency based evaluation systems. Founded in 1994, the mission of EMS has always been to provide a safe environment for healthcare professionals to develop patient safety skills.
They feel strongly that their state-of-the-art technology makes simulation training even easier, from automated training sessions, to feature-rich, interactive tools in the simulation classroom and mobile solutions for in-situ training environments. The EMS goals is to bring educators the best collaborative innovation the industry has to offer – as “innovation has been written into our DNA for over 20 years”!
Laerdal SimCapture: After acquring B-Line Medical in 2019, Laerdal relaunched the brand as audiovisual recording tools as SimCapture. SimCapture allows you to effectively manage, record, and assess simulation training, both on-site and in-situ. Capture audio, video, annotations, patient monitors, and simulator data in a single web-based interface. The solution enables medical schools, nursing schools, and hospitals to deliver high-quality training, education, and quality improvement programs. Over 500 healthcare institutions in more than 35 countries use SimCapture to generate reports and statistics on performance and trends to improve administration, track usage, and learning outcomes. And, since SimCapture is mobile-friendly, you can do this anywhere and anytime.
Sponsored Content:
Intelligent Video Solutions: With headquarters in Waukesha, Wisconsin, Intelligent Videos Solutions is an innovative software solution that empowers users to create and manage their own video databases. Founded in 2009, this powerful tool helps organizations increase the use of video to improve the effectiveness of a wide variety of programs with increased focus on medical simulation in the past several years. This unique audio visual recording and debriefing software leads users to increase the effectiveness of their programs by leveraging the power of video. With over 15 years of experience, the team at Intelligent Video Solutions is dedicated to delivering excellence and can meet any challenge. Comprised of a group of video technology professionals who are passionate about helping clients use video to advance their organizations’ purpose, Intelligent Video Solutions is unified by the goal of providing outrageous customer service.
SIMStation: As technicians, designers and enthusiasts for medical simulation, the SIMStation team see it as their job to set a new standard in the area of audio-video-debriefing with their mobile and fixed video capture and debriefing equipment. SIMStation was founded in 2011 by two collaborating professional service companies with 20 years of experience in the fields of multimedia software, broadcasting and stage media technology. They younger Vienna based company already boasts over 20 employees who design and develop their highly innovative audio-visual systems for medical simulation. The company prides itself on advising simulation and training centers on the planning and implementation of simulation-technology facilities and is extremely prevalent across Europe and the Middle East as it continues to expand globally.
KBPort: KbPort LLC is a technology solutions provider serving multiple markets with core objectives in the medical simulation space. Founded in 2005, KbPort consistently employs cutting edge technology to present learners with understandable, easy-to-navigate, realistic interfaces. The company and partners have been committed to enabling institutions to achieve exceptional educational outcomes by using the most advanced technology to offer the highest fidelity systems possible. Enhance the reality and depth of simulation based education efforts to affect a more positive educational outcome with the most powerful recorder options available from with KBPort including their ETC (Event Triggered Camera) systems and the integration capabilities of Simplicity. Available in a variety of form factors to meet the needs of any simulation environment!
Vosaic: Born out of the popular sports debriefing system Studiocode, Vosaic enables learners and their educators to record or upload videos from anywhere using their favorite devices, mark important moments on a video timeline, and leave comments on-the-spot or after the video is recorded. As well, Learners can react to feedback, make adjustments to their practice, and repeat the process as needed. Whether you’re using TeamSTEPPS or other instructional frameworks for this “performance discovery”, with Vosaic educators can easily customize what they want to mark in simulation videos for more effective debriefs. Moments marked with Vosaic are captured in full length-not just a single frame timestamp-allowing you to replay important moments in their entirety.
SMOTS (UK): Launched in 2005 with a 24 bed installation at Oxford Brookes School of Health and Social Care, SMOTS is a system of hardware and software that can easily and unobtrusively record video, audio and the vital signs readings of any medical procedure or simulation. The system records all material all of the time. This ensures that review and debrief is straightforward and when a particular clip arises that is worthy of retention for future training, it can be exported as an MPEG4 video. The SMOTS systems are widely used by dental and medical training establishments and having seen considerable success in the UK, across Europe and the Far East. Finally, the SMOTS system can also allow surgical procedures to be demonstrated to large numbers of consultants in a live operating/lecture theatre connection with no hiring in of expensive and often cumbersome video conferencing facilities.
Noldus Information Technology: Noldus Information Technology was established in 1989 by Lucas Noldus, founder and CEO of the company. With a Ph.D. in animal behavior from Wageningen University, he developed the company’s first software tool during his research in entomology. Noldus has strived to advance behavioral research ever since, evolving into a company that provides integrated systems including software, hardware, and services. They now offer a wide range of solutions for research in animal and human domains, including biology, psychology, marketing, human factors, and healthcare. Their systems have found their way into more than 9,700 universities, research institutes, and companies in almost 100 countries. Their Viso system is an easy-to-use solution for creating video and audio recordings in order to capture behaviors and interactions of your participants, and to educate, train, and improve skills of students and professionals. Their Observer XT platform is their most complete software for behavioral research which enables researchers to code behaviors on a timeline and unravel the sequence of events to integrating different data modalities in a complete lab.
B-Line Medical (Acquired by Laerdal Medical in 2019): B-Line Medical was a Washington D.C. based company that provides medical simulation centers around the world with digital recording systems and learning management solutions to enhance debriefing, which was acquired by Laerdal Medical in 2019. B-Line Medical was formed in 2005 around the development of their first product Clinical Skills, a standardized patient encounter audiovisual and management system. Since then B-Line Medical has expanded their product base to include other solutions which support learning in healthcare simulation learning environments. Their systems are used in Nursing, Medical, Allied Health, Hospitals and Military institutions around the world. Their leading product, SimCapture, allows educators to automate, track and report on every aspect of your simulation center’s activities. The simulation in healthcare LMS is the choice of over 500 healthcare institutions in 35 countries. SimCapture simultaneously simplifies and enhances program activities.
Codimg: The real value of Codimg is its ability to recognize training elements and reproduce key moments, to provide genuine and immediate debriefing. It also helps users to reinforce and mark positive areas of their training, with a better assimilation and subsequent application of what they have learned, from the perspective of passive observer. The system’s versatility and simplicity of extracting meaningful actions using Codimg’s iPad or iPhone application are other virtues highlighted by Dr. Beneharo Darias : “Once installation is complete it is simple to work with. We have been using the Codimg View application on an iPad Pro to capture video. This means instructors can use it anywhere in the medical environment – without having to ask IT for help setting up. Together with the main software, we mark the video using our own template: with customized categories and descriptors. This has replaced any type of subjective annotation in notebooks, which were being used previously, but which could not offer precise details. Through the recording of actions from various angles, we review tagged videos, comparing and organizing recorded actions.”
Nordic Simulators: Nordic Simulators is a Finnish company that develops and manufactures technological solutions for learning environments in various fields of education. The company’s product portfolio focuses on easy to use, affordable and reliable recording and debriefing systems. These systems are also well suited for smaller simulation centers and organizations. In addition to fixed recording solutions, the company specializes in flexible mobile recording & debriefing systems that enable the user to expand their available facilities by turning any room into a simulation training or debriefing space within minutes. The mobile systems are completely autonomous, easily transportable, equipped with wireless camera technology and battery powered. These features make training sessions outside in the open a possibility as well. The mobile solutions can be expanded to incorporate permanently installed hardware, turning the solution into a hybrid system that combines the best features of both mobile and fixed recording and debriefing systems. All Nordic Simulators’ recording and debriefing solutions support remote learning and teaching methods.
AV Integrators (More Information Coming Soon)
- Level 3 AV
- Ford A/V
- AVI-SPL
- Drake Systems Group
- Kontek
- More coming Shortly!
Simulation Recording Debriefing Systems Latest News

Massive Upload of Must-See IMSH 2024 Exhibitor Demo Videos

Watch These Exclusive IMSH 2024 Vendor Demos for Latest Clinical Simulation Technologies

Education Management Solution’s Training in Motion Helps You Affordably Increase Sim Utilization

Global Healthcare Simulation Industry News Update December 2023

EMS Competency Solution to Meet Nursing Education Competencies Needs

Healthcare Simulation Webinars Focused on AudioVisual Recording Systems

EMS Supercharge Your Sim with Centralized Operations, Increased Flexibility, and Actionable Data

Accreditation Council for Education in Nutrition and Dietetics (ACEND) Tracks Competencies with Comptency.AI

Watch All #IMSH2023 Healthcare Simulation Industry Press Box Interviews

IMSH 2023 Vendor Demos: CAE Healthcare, EMS, Laerdal, SimX, Sentinel U and Medical Shipment

EMS Launches Intelligent Immersive Reality Learning Solution

IMSH 2023: Healthcare Simulation Vendor Updates

Exclusive: Education Management Solutions New CEO Matthew Merino Shares Vision for Healthcare Simulation Industry

New CAE LearningSpace Launches Offer Next-Level Clinical Simulation Solutions
Sponsored Content: