SimGHOSTS
SimGHOSTS, also known as The Gathering Of Healthcare Simulation Technology Specialists, is an international United States-based non-profit organization. The organization is dedicated to supporting individuals and institutions operating medical simulation technology and spaces through hands-on training events, online resources and professional development.
About SimGHOSTS
By offering support and resources to medical simulation professionals, SimGHOSTS hopes to create a healthcare education culture where people are empowered to use simulation technology to improve learning and patient care outcomes. For this reason, SimGHOSTS has created six core values, the first of which is to innovate the world of healthcare simulation and patient safety.
Sponsored Content:
Other organizational core values include advocating for those operating healthcare simulation technology spaces, educating the professional community to improve outcomes and networking with global community members at regional events and online hubs. The last two core values are to engage champions, institutions and organizations, and zeal for the craft of simulation in healthcare throughout the community and profession.
Enacting these values, SimGHOSTS has formalized a strategic direction the organization plans to take in the coming years. This plan encompasses a sustainability approach: striving for operational excellence and ensuring financial stability. The plan also includes growth and development, community, professional development and collaboration standards that create mutual value. This strategic plan was developed in consultation with the SimGHOSTS board of directors early in 2019, and serves to document the strategic direction and goals for the organization for the three year period concluding at the end of 2021.
Demonstrating the success of SimGHOSTS thus far, the organization continues to bring in record-breaking attendance at their annual hand-on training symposium conferences. As of 2019, over 2,000 simulation champions attended events all over the world. In addition to the annual event, SimGHOSTS also provides insight and information on a daily basis through the organization website. There are currently over 3,000 online subscribers to the website gaining access to courses, books, forum discussion boards and more!
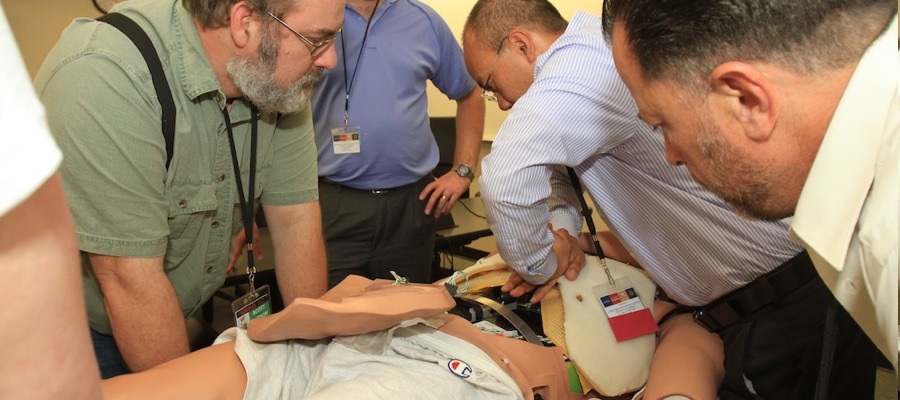
SimGHOSTS events provide hands-on training workshops, special pre-symposium courses and podium presentations in manikin programming and hardware repair; A/V system design, integration and consolidation; IT networking and debugging; trauma and suturing moulage makeup; video production and editing techniques; team communication and leadership; medical pharmacology for scenarios; career development and staff management; virtual reality (VR) and augmented reality (AR) and more.
Sponsored Content:
Anyone responsible for the technical operation of a medical simulation lab, including Sim Techs or clinical educators tasked with operating the day-to-day of simulation spaces, will find these events highly relevant. Additionally, anyone evaluating medical-simulation based technology should strongly consider attending one of these events, as most major industry vendors are encouraged to attend.
History of SimGHOSTS
The Gathering of Technicians, or GOT SIM, was founded in 2011 by Lance Baily, the founding Director of the Clinical Simulation Center of Las Vegas (CSCLV) for the Nevada System of Higher Education. Baily got his start in healthcare simulation as a simulation technology specialist for the Los Angeles Community College District before being hired to manage the CSCLV.
Focusing on the realm of healthcare simulation, Baily began to combine his love of computer technology, programming, audio video production, experiential learning and Fire/EMS healthcare training into an online niche. Having traveled the world touring healthcare simulation labs and attending healthcare simulation meetings, Baily wanted to do more to support the unique multifaceted profession of being a “Healthcare Simulation Technology Specialist.”
Entering into the second year, the GOT SIM meeting became an official non-profit organization after changing the meeting’s name to SimGHOSTS, or “The Gathering Of Healthcare Simulation Technology Specialists.” Additional support for the formation and operation of this new annual meeting to continue outside of the CSCLV has also come from Kam McCowan and John Cordova, and had founding sponsorship from B-Line Medical and Pocket Nurse.
The event moved to the San Antonio College School of Nursing and Allied Health Building in year three, with coordination provided by Simulation Technician, Joe Crain. Then, in late 2013, the organization was approved as a tax-exempt 501(c)3 educational based charitable entity by the US Federal IRS. This meant SimGHOSTS could continue pursuing the mission to provide educational support to Sim Techs, apply for federal grants and to receive charitable donations.
Even more recently, in 2014, SimGHOSTS repeated the now famous North American event at the American College of Chest Physicians, and successfully added another international event in Australia. Hosted by the University of the Sunshine Coast, SimGHOSTS was praised as an event dedicated to supporting those who operate simulation technologies. Furthermore, SimGHOSTS signed the first affiliation agreement with UK’s Association for Simulated Practice in Healthcare (ASPiH) in 2014 as well. This is where the developmental stages and planning for a jointly operated third international SimGHOSTS UK were announced.
Then, in 2015 the Symposiums continued to expand taking place across the globe with two new locations: Dubai and the United Kingdom. These expansions were largely thanks to support from Simulead and the SimGHOSTS partnership with the ASPiH. This year also saw the launch of another much anticipated online course program in simulation.
In 2016, SimGHOSTS focused specifically on the events held within the United States, United Kingdom and Australia. Supporting over 350 Simulation champions around the world, SimGHOSTS simultaneously launched a new website to connect the global community together through discussion groups, courses and recorded sessions. Through these accomplishments, SimGHOSTS became affiliated with major international simulation and healthcare organizations, including SSH, INACSL, GNSH, HIMSS, IPSS, Simulation Australia, ASPiH and more.
In 2017, SimGHOSTS hosted their seventh annual United States event at the WakeMed Center for Innovative Learning with Dr. Amar Patel, as well as simulation technology training tracks for the SESAM Paris event and SingHealth Singapore S3 Event. The organization also affiliated with GNSH, SimOne and PASSH. The following year, in 2018, SimGHOSTS held meetings for the United States at the University of Tennessee Health Sciences Center and in Australia at the University of the Sunshine Coast, in partnership with Simulation Australasia, ASSH and Serious Games Australia. Each event had a record-breaking attendance within the respective region.
Most recently, SimGHOSTS held a United States event at Florida International University’s Nicole Wertheim College of Nursing and Health Sciences Simulation Teaching and Research (STAR) Center, as well as provided international events in Singapore and Argentina. Visit the SimGHOSTS website for the latest updates!
Gathering of Healthcare Simulation Technology Specialists Latest News

Next Month’s International Healthcare Simulation Congress in Argentina Looks to Impress

Global Medical Simulation News Update March 2024

How to Fill-in for the Role of Clinical Simulation Technician

Global Healthcare Simulation News Update January 2024

SimGHOSTS 2023 Hosted at UNMC iEXCEL: One of World’s Best Healthcare Simulation Centers
How to Impact Clinical Outcomes as a Healthcare Simulation Technology Specialist

UPMC’s WISER Academy Offers Unique Clinical Simulation Professional Development Opportunities

SimGHOSTS Shares Updates, Upcoming Conference Information

Free Online IT Training Courses for Healthcare Simulation Technology Specialists

Watch All #IMSH2023 Healthcare Simulation Industry Press Box Interviews

Additional #IMSH2023 Press Box Interviews with Key Healthcare Simulation Industry Leadership

Looking Ahead: 2023 Healthcare Simulation Events
Sponsored Content:
















